Antimicrobial R esistance P atterns in E xtended - spectrum ÃÆà ½Ãâò - lactamase P roducing Klebsiella pneumoniae I solates in a Razi Hospital Marand, Iran
Abolfazl Jafari Sales , Behboud jafari , Najiyeh beygoli
1Young Researchers and Elite Club,Ahar Branch,Islamic Azad University,Ahar,Iran;
2Central Medical Laboratory of Tabriz,Tabriz,Iran.
- Corresponding Author:
- Abolfazl Jafari Sales
Tel: +98 (0)914-7611841
Fax: +98 (0)414-2262359
E-mail: a.jafari_1392@yahoo.com
Abstract
The prevalence of antibiotic resistance among extended-spectrum β-lactamase (ESBL)-producing Klebsiella pneumoniae has increased markedly in recent years. This could be attributed to association of multi drug resistance in ESBL producing isolates. The present study was aimed to determine the antimicrobial resistance profile of ESBL producing Klebsiella pneumoniae isolates from various clinical samples. In this study,250 cases of Klebsiella pneumoniae within 9 months from patients referring to Razi Hospital Marand were collected and identified by biochemical tests. ESBL screening and confirmation along with antimicrobial resistance test was done according to the Clinical Laboratory Standards Institute (CLSI) guidelines. Of the 250 isolates, 150 (60%) were identified as having ESBL phenotype. Over 100% of ESBL isolates showed resistance to Ceftazidime and least resistance was found to Meropenem (3.3%). The prevalence of ESBL is increasing day by day in nearly every center of different countries and necessary steps to prevent the spread and emergence of resistance should be taken.
Keywords
Klebsiella pneumonia ,Extended Spectrum Beta Lactamase,Antimicrobial resistance.
1. Introduction
Certainly,modern medicine is indebted to developments in antibiotics research areas and antibiotics,by treating and elimination of infectious agents play a critical role in survival and increased quality of life [1]. The precise definition of the term Extended-Spectrum β-Lactamase (ESBL) remains unclear but is generally used to refer to any β-lactamase,'generally acquired rather than inherent to a species,that is either able to confer resistance to oxyimino-cephalosporins (but not carbapenems),or that has an increased ability to do so,as compared with classic members of its genetic family [2]. ESBL producing strains of Enterobacteriaceae have emerged as a major problem in hospitalized as well as community based patients [3]. These organisms are responsible for a variety of infections like urinary tract infection (UTI),septicemia,hospital acquired pneumonia,intra-abdominal abscess,brain abscess and device related infections. Organisms producing ESBLs are clinically relevant and remain an important cause of failure of therapy with cephalosporins [4]. ESBLs are primarily produced by the Enterobacteriaceae family,in particular Klebsiella pneumoniae and Escherichia coli [5]. Bacteria harboring ESBLs may also acquire and most often exhibit additional resistances to other antimicrobial classes such as the quinolones,tetracyclines,cotrimoxazole,trimethoprim,and aminoglycosides,which further limits therapeutic options and thus pose a therapeutic dilemma [6-9]. ESBL - producing K. pneumoniae strains have been implicated in numerous outbreaks of nosocomial infections over the last two decades [10,11]. Considering the extensive use of β-lactam antibiotics including third - generation cephalosporins for the treatment of both hospital - and community - acquired infections in Iran,prevalence of ESBL positive clinical isolates is very probable. A single report on these resistant bacteria from Iran denoted the occurrence of K. pneumoniae producing ESBL as high as 44.5% [12]. In this study,we determined the prevalence of ESBL production among K. pneumoniae isolated from inpatients,their susceptibility patterns,as well as the risk factors associated with the acquisition of these isolates. Today,there is a concern about the spread of such bacteria from hospital to community [13]. Current knowledge of prevalence of ESBL production by commonly isolated organism such as K. pneumoniae is necessary to understand the disease burden and to take necessary action to prevent the spread. Therefore the present study was conducted with an objective to find out the prevalence of ESBL producing K. pneumoniae and its antimicrobial resistance profile to formulate effective antibiotic strategy and plan a proper hospital infection control strategy to prevent the spread of these strains.
2. Methods
This descriptive cross sectional study,for a period 9 months (from December to August of 2013) on 250 strains of K. pneumoniae isolated from clinical samples (blood and urine) of Razi Hospital Marand was isolates ,and after test biochemical ,All these isolates were subjected to antibiotic susceptibility testing and studied for extended-spectrum β- lactamase production according to the National Committee for Clinical Laboratory Standards Institute(CLSI). The results were interpreted according to the current guidelines of the CLSI [14]. The following antibiotics were tested: amikacin (30 μg),cefixime (5μg),cefotaxime (30 μg),ceftazidime (30 μg),cefuroxime (30 μg),ciprofloxacin (5 μg),coamoxiclav (20/10 μg),co-trimoxazole (1.25/23.75 μg),gentamicin (10 μg),meropenem (10 μg),nalidixic acid (30 μg),itrofurantoin (300 μg),norfloxacin (10 μg) and piperacillin/tazobactam (100/10 μg) were placed on the Mueller-Hinton agar plates and incubated at 37°C overnight. After overnight incubation,the diameter of each zone of inhibition was measured in mm. The screening test in order to identify bacteri a producing ESBLs in accordance with the instructions NCLS,using the disc antibiotics ceftazidime (CAZ 30μg) and cefotaxime (CTX 30μg) in combination with clavulanic acid (CLA 10μg) ( CinnaGen,Iran) was conducted. The standard strain,Klebsiella pneumoniae ATCC 700603 as a positive control and Escherichia coli ATCC 25922 was used as a negative control [15]. The collected data were statistically analyzedusing SPSS version 18 Svrt. p<0/05 was considered statistically significant.
3. Results and Discussion
In this study antibiotic resistance patterns 250 K. pneumoniae strains isolated from patients referred to Razi Hospital Marand city,compared to 10 antibiotics were determined using DAD (Disk Agar Difusion). Samples were collected from 139 (55.6%) females and 111 (44.4%) males. Of the 250 K. pneumoniae isolates,150 (60%) ESBL K. pneumoniae isolated and 100(40%) non-ESBL producing K. pneumoniae isolated. The result of ESBLand non-ESBL producing K. pneumoniae recovered from urineand blood given in Table1.
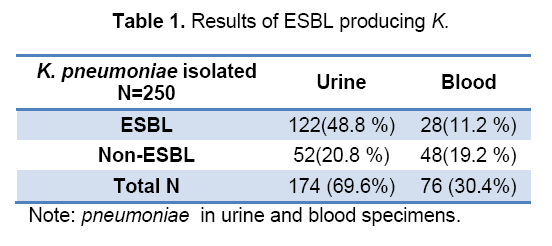
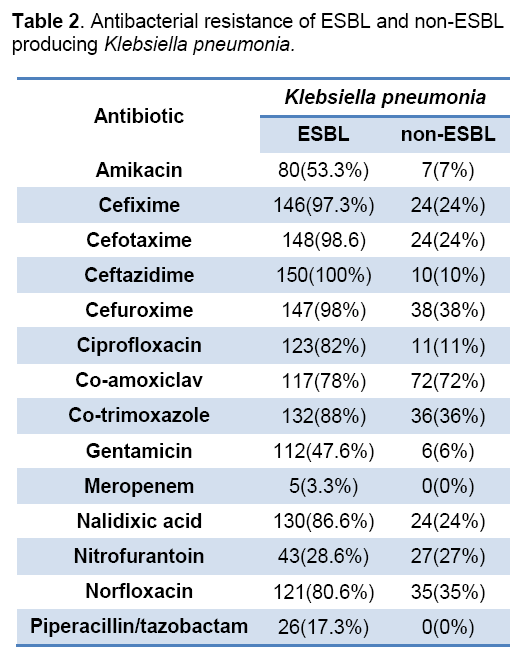
The mean age of patients was 65.42 ± 19 years . 58% of ESBL-producing isolates were from females And 42% isolates from males. In 10 of the antibiotic resistance of greater than 50% is observed. This differenceis meaningful. High-level resistance was for Ceftazidime (100%) and least resistance was found to Meropenem (3.3%) (Table 2).
The discovery and development of antibiotics was undoubtedly one of the greatest advances of modern medicine. Unfortunately the emergence of antibiotic resistance bacteria is threatening the effectiveness of many antimicrobial agents. Beta– lactamase is the main defending system of gramnegative bacteria against β-lactam antibiotics. Since the first time β-Lactam antibiotics were used,Beta– lactamases evolved simultaneously and they played a major role in treatment failure [16]. Increased outbreak of antibiotic-resistant microorganisms such as extended spectrum beta–lactamase producing gram-negative bacteria among sensitive patients has resulted in spread of dangerous infections . Resistance and transmission of resistant bacteria occurs because of the pressure of improper use of selected antibiotics . The resistant bacteria are highly prevailed,which is most importantly due to over prescription,prescription of inadequate doses of medication,inappropriate treatment,and wrong diagnosis of infectious bacteria by laboratories followed by inappropriate choice of antibiotics for healing or unreliable antibiograms . In the present study,an attempt was made to understand the prevalence of ESBL producing Klebsiella pneumonia. The emergence and spread of ESBLproducing bacteria appear to be mostly caused by the the widespread use of broad-spectrum beta-lactam drugs. So that nowadays,we are witnessing the increasing rate of the bacteria in different parts of our Hospital. Prevalence of extended spectrum beta–lactamases in Klebsiella sp. and Escherichia coli are reported to be 19% and 4%,respectively (SENTRY Antimicrobial Surveillance,2000) [17,18]. In a study conducted in Seoul hospitals in 1993-98,it was revealed that strains of Klebsiella pneumoniae and Escherichia coli extracted from blood cultures of children produced ESBL (17.9% and 52.9%,respectively) [19]. Another study in 2003 on urine cultures of patients in ICU wards suggested that 25.6% of strains of Klebsiella pneumoniae and Escherichia coli produced ESBL [17]. Prevalence of ESBLs is reported to be 6% and 87% in India [18,20,21]. These enzymes are also observed in European countries. For example,its prevalence it French hospitals is 40% [17]. Highest outbreak of ESBL from Klebsiella pneumoniae were in Western Pacific region (Latin America) (45.4%),Europe (22.6%),United States (7.6%) and Cananda (4.9%) [22].
In the Middle East,where Iran is located,prevalence of ESBL-producing K. pneumoniae is as follows: Saudi Arabia (2005) 12.2% [23],Lebanon (2003) 20.0% [24],Egypt (2004) 37.5% [25],Turkey (2004) 50.0% [26],and Jordan (200) 80% [27]. In Pakistan (2005),a study performed in Karachi showed an ESBL prevalence of 36.0% in nosocomial K. pneumoniae isolates [28]. A higher rate was reported from India where 80.0% of K. pneumoniae isolates in a tertiary care center were labeled as ESBL producers [29]. In the present study the ESBL producing K. pneumoniae were 60%,respectively. In studies performed throughout the world,the frequency of ESBL positive K. pneumoniae was from 17% to 66.7% [30-37]. For example,in United Arab Emirates (2008),out of 130 samples,42% of K. pneumoniae were ESBL positive [33]. In Turkey (2006),47% of K. pneumoniae were ESBL positive [36]. the percentage of K. pneumoniae was similar to our study In Tanzania (2009),63%of K. pneumoniae were ESBL positive and the percentage of K. pneumoniae was similar to our study [35]. In Skopje (2009),24.3% of K. pneumoniae were ESBL positive and this percentage was Differently to our study [30]. In India (2007),out of 2655 samples,26.6% of K. pneumoniae were ESBL positive and this percentage was lower than our study which can be due to differences in test method,the type of samples and the study population [37]. ESBL producing K. pneumoniae showed higher resistance to ceftazidime (100%),cefotaxime (98.6%) and cefuroxime (98%) while lower resistance was seen with meropenem (3.3%),piperacillin/tazobactam (17.3%),and nitrofurantoin (28.6%). In a study conducted in Saudi Arabia (2005),ESBL producing K. pneumonia showed higher resistance to ceftriaxone while lower resistance was seen with meropenem (4.2%),amikacin (6.3%) and imipenem (8.3%) [38]. Kadar and Angamathu (2005) reported 11% resistance of meropenem which is more than seen in the present study [39]. One of the most striking findings of the present study was the high prevalence of resistant strains among ESBL-producing K. pneumoniae to piperacillin/tazobactam. Another study group from Iran reported 33% resistance to this antibiotic combination,which was Much more than our finding [12].
4. Conclusions
Finally,the present study showed high prevalence of ESBL-producing K. pneumoniae in our region . Determination of resistant patterns can help us to choose the best antibiotics in such a situation. Also there is a need to emphasize on the rational use of antimicrobials to decrease the spread of ESBL producing bacteria.
Acknowledgments
We would like to thank the Razi hospital and Department of Microbiology,Islamic Azad University Marand,Tabriz for their laboratory equipment and technical support.
References
- Rice LB. (2008). Federal funding for the study of antimicrobial resistance in nosocomial pathogens: no ESKAPE. J. Infect. Dis. 197(8): 1079-1081.
- Livermore DM. (2008). Defining an extended-spectrum beta-lactamase. Clin. Microbiol. Infect . 14 Suppl 1: 3-10.
- Rodriguez-Bano J,Navarro MD,Romero L,Martinez-Martinez L,Muniain MA,Perea EJ,Perez-Cano R,Pascual A. (2004). Epidemiology and clinical features of infections caused by extended-spectrum beta-lactamase-producing Escherichia coli in nonhospitalized patients. J. Clin. Microbiol. 42: 1089-1094.
- Bradford PA. (2001). Extended-spectrum beta-lactamases in the 21st century: characterization,epidemiology,and detection of this important resistance threat. Clin. Microbiol. Rev. 14: 933-951.
- Paterson DL,Bonomo RA. (2005). Extended-spectrum beta-lactamases: a clinical update. Clin. Microbiol. Rev. 18: 657-686.
- Chopra I,Schofield C,Everett M,O'Neill A,Miller K,Wilcox M,Frere JM,Dawson M,Czaplewski L,Urleb U,Courvalin P. (2008). Treatment of health-care-associated infections caused by Gram-negative bacteria: a consensus statement. Lancet. Infect. Dis. 8: 133-139.
- Morosini MI,Garcia-Castillo M,Coque TM,Valverde A,Novais A,Loza E,Baquero F,Canton R. (2006). Antibiotic coresistance in extended-spectrum-beta-lactamase-producing Enterobacteriaceae and in vitro activity of tigecycline. Antimicrob. Agents. Chemother. 50: 2695-2699.
- Pitout JD,Laupland KB. (2008). Extended-spectrum beta-lactamase-producing Enterobacteriaceae: an emerging public-health concern. Lancet. Infectz. Dis. 8:159-166.
- Talbot GH. (2008). What is in the pipeline for Gram-negative pathogens? Expert Rev Anti Infect Ther. 6: 39-49.
- Tzelepi E,Magana Ch,Platsouka E,Sofianu D,Paniara O,Legakis NJ,et al. (2003). Extended - spectrum β - lactamase types in Klebsiella pneumonia and Escherichia coli in two Greek hospitals. Int. J. Antimicrob. Agents. 21: 285-288.
- Hirakata Y,Matsuda J,Miy azaki Y,Kamihira S,Kawakami S,Miyazawa Y,et al. (2005). Regional variation in the prevalence of extended - spectrum β – lactamase - producing clinical isolates in the Asia - Pacific region (SENTRY 1998 - 2002). Diagn. Microbiol. Infect. Dis. 52: 323-329.
- Feizabadi MM,Etemadi G,Yadegarinia D,Rahmati M,Shabanpoor S,Bokaei S. (2006). Antibiotic-resistance patterns and frequency of extended - spectrum β-lactamase producing isolates of Klebsiella pneumonia in Tehran. Med. Sci. Monit. 12: BR362-365.
- Al –Jasser AM. (2006). Extended-spectrumbeta-lactamases (ESBLs): a global problem. Kuwait. Med. J. 38(3): 171-185.
- Lavigne JP,Bouziges N,Chanal C,Mahamat A,Michaux- Charachon S,Sotto A. (2004). Molecular epidemiology of Enterobacteriaceae isolates producing extended-spectrum betalactamases in a French hospital. J. Clin. Microbiol. 42: 3805-3808.
- Pannika RN,Tansawai U,Boonkerd N,Polwichai P,Dejsirilert S. (2008). Dissemination of extended-spectrum β-lactamase producing Klebsiella pneumoniae and Escherichia coli in Thai hospitals. J. Infect. Chemother. 14: 404-408.
- Fang H,Ataker F,Hedin G,Dornbusch K. (2008). Molecular epidemiology of extended-spectrum beta-lactamases among E. coli isolates collected in a Swedish hospital and its associated health care facilities from 2001 to 2006. J Clin Microbiol. 46: 707-712.
- Mendelson GV,Hait J,Ben-Israel D,Gronich E,Granot R. (2005). Prevalence and risk factors of extended-spectrum betalactamase- producing Escherichia coli and Klebsiella pneumonia in an Israeli long-term care facility. Eur J Clin Microbiol Infect Dis. 24: 17-22.
- Gordon KA,Jones RN,and the SENTRY Participant Groups (Europe,Latin America,North America). (2003). Susceptibility patterns of orally administered antimicrobials among urinary tract infection pathogens from hospitalized patients in North America: comparison report to Europe and Latin America. Results from the SENTRY Antimicrobial Surveillance Program. Diagn Microbiol Infect Dis. 45: 295-301.
- Kim YK,Pai H,Lee HJ,Park SE,Choi EH. (2002). Bloodstream infections by extended-spectrum beta-Lactamas eproducing Escherichia coli and Klebsiella pneumoniae in children: epidemiology and clinical outcome. Anti Microb Agent Chemother. 46(5): 1481-1491.
- Agraval P,Ghush A,Agrawal P,Ghosh AN,Kumar S,Basu B,et al. (2008). Prevalence of extended-spectrum beta-lactamase among Escherichia coli and Klebsiella pneumonia in Isolates in a tertiary care hospital. Indian J Path Microbiol. 51(1): 137-142.
- Manchanda V. (2005). Phenotipic characteristic of clinical isolates of Klebsiella pneumoniae evaluation of available techniques for detection of extendedspectrum β-lactamase. Indian J Med Res. 122: 303-307.
- Goosens H. (2001). MISTIC program. Summary of a European data from 1997-2000. Diag Microb Infect Dis. 41: 183-189.
- Kader AA,Kumar A. (2005). Prevalence and antimicrobial susceptibility of extended-spectrum β-lactamase-producing Escherichia coli and Klebsiella pneumoniae in a general hospital. Ann. Saudi. Med. 25: 239-242.
- Daoud Z,Hakime N. (2003). Prevalence and susceptibility patterns of extended-spectrum betalactamase-producing Escherichia coli and Klebsiella pneumoniae in a general university hospital in Beirut,Lebanon. Rev. Esp. Quimioterap. 16: 233-238.
- Bouchillon SK,Johnson BM,Hoban DJ,Johnson JL,Dowzicky MJ,Wu DH,Visalli MA,Bradford PA. (2004). Determining incidence of extended spectrum β-lactamase producing Enterobacteriaceae,vancomycin-resistant Enterococcus faecium and methicillin-resistant Staphylococcus aureus in 38 centres from 17 countries: the PEARLS study 2001-2002. Int. J. Antimicrob. Agents. 24: 119-124.
- Yaman A,Tasova Y,Kibar F,Inal AS,Saltoglu N,Buyukcelik O,Kurtaran B,Dundar IH. (2004). Investigation of the antibiotic susceptibility patterns of pathogens causing nosocomial infections. Saudi. Med. J. 25: 1403-1409.
- Shehabi AA,Mahafzah A,Baadran I,Qadar FA,Dajani N. (2000). High incidence of Klebsiella pneumoniae clinicalisolates to extended-spectrum β-lactam drugs in intensive care units. Diagn. Microbiol. Infect. Dis. 36: 53-56.
- Jabeen K,Zafar A,Hasan R. (2005). Frequency and sensitivity pattern of Extended Spectrum Beta Lactamase producing isolates in a tertiary care hospital laboratory of Pakistan. J. Pak. Med. Assoc. 55: 436-439.
- Mathur P. Kapil A,Das B,Dhawan B. (2002). Prevalence of extended spectrum β-lactamase producing Gram-negative bacteria in a tertiary care hospital. Indian. J. Med. Res. 115: 153-157.
- Kaftandzhieva A,Kotevska V,Jankoska G,et al. (2009). Extended-spectrum betalactamase- producing E. coli and Klebsiella pneumoniae in children at University pediatric clinic in Skopje. Macedonian. J. Med. Sci. 2(1): 36-41.
- Wani KA,Thakur MA,Siraj Fayaz A,et al. (2009). Extended spectrum Betalactamase mediatedresistance in Escherichia coli in a tertiary care hospital. Int. J. Health. Sci. (Qassim). 3(2): 155-163.
- Ling TK,Xiong J,Yu Y,et al. (2006). Multicenter antimicrobial susceptibility survey of gram-negative bacteria isolated from patients with community-acquired infections in the People's Republic of China. Antimicrob. Agents. Chemother. 50(1): 374-378.
- Al-Zarouni M,Senok A,Rashid F,et al. (2008). Prevalence and antimicrobial susceptibility pattern of extendedspectrum beta-lactamase-producing Enterobacteriaceae in the United Arab Emirates. Med. Princ. Pract. 17(1): 32-36.
- Mshana SE,Kamugisha E,Mirambo M,et al. (2009). Prevalence of multiresistant gram-negative organisms in a tertiary hospital in Mwanza,Tanzania. BMC. Res. Notes. 2(1): 49.
- Abdel-Hady H,Hawas S,El-Daker M,et al. (2008). Extended-spectrum betalactamase producing Klebsiella pneumoniae in neonatal intensive care unit. J. Perinatol. 28(10): 685-690.
- Ozgunes I,Erben N. Kiremitci A,et al. (2006). The prevalence of extended-spectrum beta lactamase-producing Escherichia coli and Klebsiella pneumoniae in clinical isolates and risk factors. Saudi. Med. J. 27(5): 608-612.
- Shahid M,Malik A,Akram M,et al. (2008). Prevalent phenotypes and antibiotic resistance in Escherichia coli and Klebsiella pneumoniae at an Indian tertiary care hospital: plasmid-mediated cefoxitin resistance. Int. J. Infect. Dis. 12(3): 256-264.
- Zahran,AJ,Akhtar N. (2005). Susceptibility Patterns of Extended-Spectrum ß- Lactamase (ESBL)-producing Escherichia coli and Klebsiella pneumoniae isolated in a teaching hospital. Pak. J. Med. Res. 44(2): 64-67.
- Kadar AA,Angamathu K. (2005). Extended-spectrum beta-lactamases in urinary isolates of Escherichia coli,Klebsiella pneumoniae and other gram-negative bacteria in a hospital in Eastern Province,Saudi Arabia. Saudi. Med. J. 26(6): 956-959.

Open Access Journals
- Aquaculture & Veterinary Science
- Chemistry & Chemical Sciences
- Clinical Sciences
- Engineering
- General Science
- Genetics & Molecular Biology
- Health Care & Nursing
- Immunology & Microbiology
- Materials Science
- Mathematics & Physics
- Medical Sciences
- Neurology & Psychiatry
- Oncology & Cancer Science
- Pharmaceutical Sciences
